
Skin care for your legs
How to care for your veins and skin
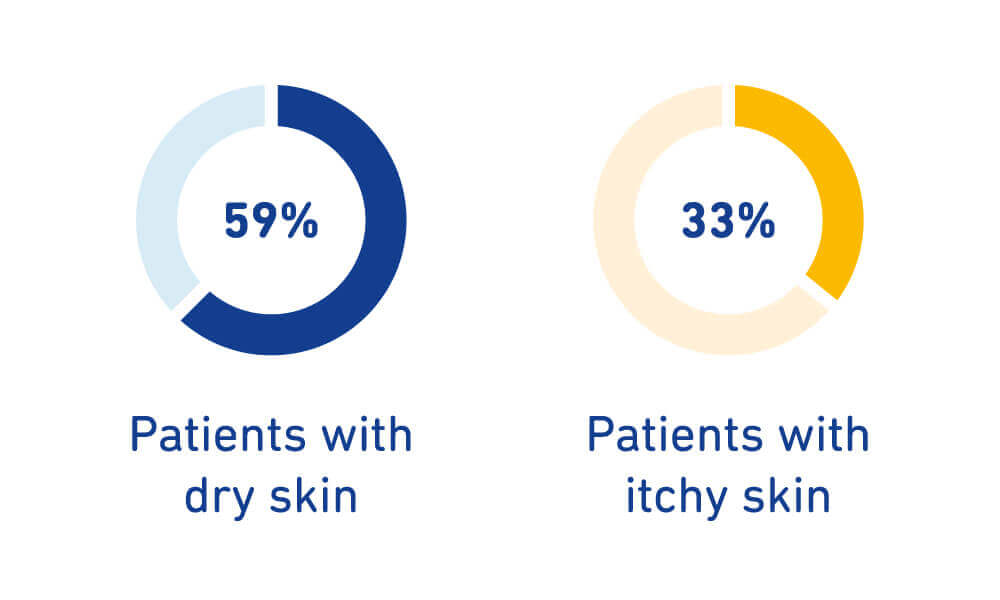
Medical compression stockings are an important part of treating vein problems. They can be, however, slightly challenging for the legs’ skin. More than half of patients who regularly wear medical compression stockings battle with dry skin. If a lack of skin moisture makes the legs flaky or causes itching, some people avoid wearing the stockings even though they are so beneficial. It’s understandable: for those with a tendency to get dry skin, wearing the stockings can become unpleasant quickly because they lie close to the skin so they can exert the required therapeutic pressure from the outside. In cases of certain vein problems, the skin doesn’t get supplied with enough nutrients, which also leads to dryness. If medical compression stockings are indispensable for medical reasons, however, luckily, there are solutions. It’s important to understand how a lack of moisture develops in the skin and what you can do about it.
What does “dry skin” mean?
Healthy skin is coated in a thin film of moisture. It contains minute droplets of fat – known as the body’s own lipids – and other moisture-retaining factors. This film keeps the skin smooth and protects it from pathogens and environmental influences. The condition is called dry skin when this hydrolipid film is insufficiently developed. This will become particularly problematic if tiny cracks form or areas become sore. This means that bacteria, fungi, or chemical substances can get into the skin and cause inflammation or irritation there. Similarly, dry skin can cause a rash or eczema.
How to identify dry skin?
Dry skin mainly manifests with visible skin flakes occurring in the areas where the skin has dried out. Healthy skin, too, is coated in dead skin cells that form the stratum corneum, the corneal layer of the skin. If the moisture film is intact, they are not visible: the thin hydrolipid film consisting of water, fat droplets, and dissolved substances keeps the callous flakes together that lie on top of each other like tiles. This ensures an even, smooth skin texture. The film is thus a working protective barrier against external influences. Where the skin has become dry, however, this connective material is missing, meaning the callous flakes loosen, and moisture can evaporate from the skin. In areas where the skin has lost its moisture balance, the skin flakes come off in large quantities and are visible as a white layer. Itching and taut or red skin is also an indication of dryness and a sign of local irritation caused by environmental influences or microorganisms.
How does dry skin develop?
The skin’s hydrolipid film is often impaired by an interaction of individual factors and environmental influences. Predisposition – i.e. a certain skin type – plays an important part in this. Some people tend to get dry skin more than others. The sebaceous glands in their skin produce less fat, meaning that dry skin occurs on relatively minor occasions or seemingly without any reason.
But even a functioning, well developed hydrolipid film can be weakened by the following factors:
Dry skin can also be caused by various conditions, such as diabetes, neurodermatitis, hypothyroidism, allergies, or problems with the gastrointestinal tract. Certain vein problems, such as chronic venous insufficiency (CVI), go hand-in-hand with an insufficient supply to the skin, which, in turn, leads to dry skin. Owing to hormonal changes, dry skin can also increasingly occur during pregnancy and later on in life.
Note:
Dry skin is not just a cosmetic problem. It can be an indication of various minor but also severe conditions, such as chronic venous insufficiency. Keep a close eye on your skin and consult a physician in case of irregularities.
What does dry skin affect the legs?

Skin regions with less circulation and fewer sebaceous glands are particularly at risk from drying out. The sebaceous glands’ fat production is reduced. Therefore fewer nutrients are available for the development of the hydrolipid film. This affects the lower legs, in particular, but also the ankles and knees, as well as the feet.
In cases of vein problems, an additional factor is that the skin on the legs is not supplied with sufficient nutrients, which also leads to dry skin. Medical compression stockings that help in cases of vein problems are a little tighter on the skin than conventional stockings – as a function of their therapeutic effect. Wearing them may be uncomfortable in cases of dry skin – but it certainly shouldn’t stop you! The answer is ensuring good skin care.
What can you do about dry skin?
In general, the following applies: in order to keep the hydrolipid layer of the skin functioning, regular skin care and a healthy diet with sufficient liquids are indispensable. This provides the necessary elements for the protective layer from the inside and the outside. Additionally, areas of dry skin should be moisturized several times per day using care lotions. They will provide the necessary moisture-retaining factors and support the skin in restoring its protective film.

What skin care is suitable for those wearing medical compression stockings?
You can effectively prevent itchy legs and dry skin caused by medical compression stockings by caring for your skin as required. Before putting on the stockings, you can use a special care foam, for example. Bauerfeind care foam provides gentle care that improves your skin without being oily. The resulting protective film even makes it easier to put on your medical compression stockings. You can also use the foam after wearing the stockings for an additional boost of protection and care. What’s more, Bauerfeind care foam is particularly suitable for the needs of those suffering from allergies or diabetes.
For dry and sensitive skin, VenoTrain® LOTION is highly suitable. It was developed in cooperation with Sebapharma. It’s a light, yet effective lotion you can use in the evening to ensure the perfect care of your legs when you’ve been wearing your medical compression stockings during the day. It provides moisture, creates more skin elasticity, stabilizes the acid protective layer, and reduces itching and feelings of taut skin.
How can medical compression stockings help in cases of dry leg skin?

In addition to you applying moisturizer to your skin, it’s ideal, of course, for your medical compression stocking itself to provide skin care. And this is exactly what the VenoTrain® cocoon does: the knitted fabric features special fibers – the cocoon care threads – that contain lipid depots. During direct contact with the skin, these lipids are released and continuously dispensed to the skin. The outer skin layers thus receive the required elements to keep the hydrolipid film intact, therefore preventing the skin from drying out. Wearing the VenoTrain® cocoon also helps maintain the barrier function of the skin by preventing rough skin and preserving the skin’s moisture.
Thanks to these nurturing qualities, this special compression stocking guarantees excellent wearing comfort because itching or irritation caused by dry skin is much more rare. The clinically tested lipid care complex keeps your skin smooth, provides it with the necessary care substances, and calms it. Your skin is cared for even while you are wearing the VenoTrain® cocoon stockings. The compression effect then ensures the ideal venous return flow in the legs, which supports the supply to the skin from the inside.
RETAILER SEARCH
Get advice on site!
Find a suitable retailer near you.
